Healthcare is an industry for which rapid implementation of innovations is as necessary as air and, at the same time, one where these innovations most often pass with pain and misery. The entire hefty system has long needed reform, but change has been too slow. The new touchstone is believed to be COVID-19. The scope of the disaster forced many medical institutions to change their work processes to help significantly increased patient flow effectively.
One option for dealing with the epidemic was Agile. This methodology’s flexibility has helped significantly improve and streamline the interaction between doctor and patient, medical center, hospital, and pharmacy.

What is Agile?
The term Agile came to healthcare and other industries from the IT field – from the need to smooth workflows in software development. About a quarter of a century ago, developers used the methodology of Waterfall, where the second part of the team could not start working until the first part was ready. Constant downtime did nothing to improve productivity.
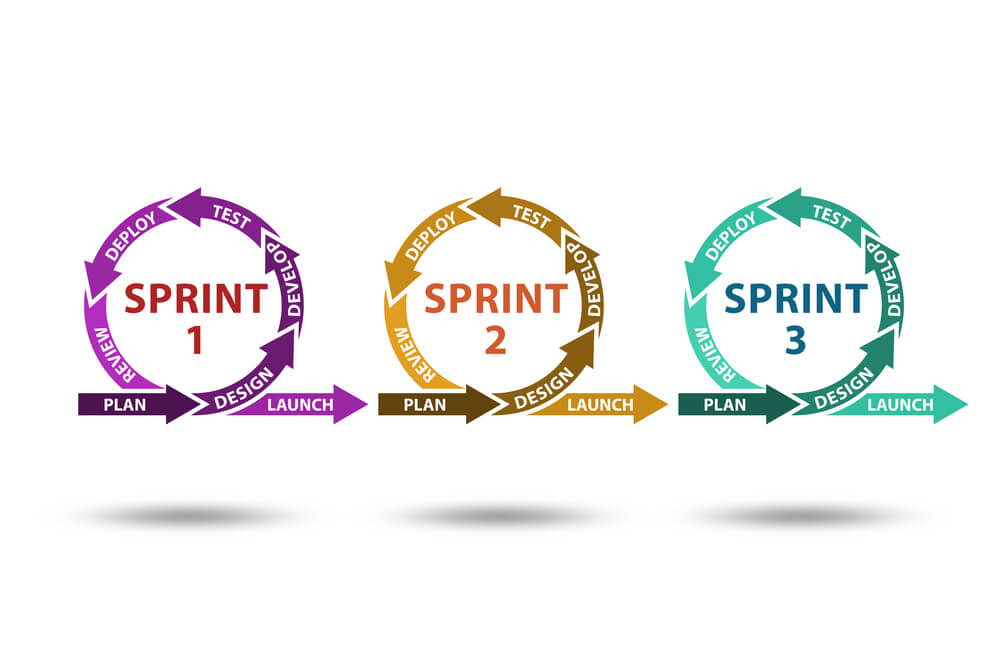
Agile is a kind of team approach to project management. It is designed to increase team productivity by doing the work in small repetitive parts – sprints (usually a two-week period with specific goals and objectives, but iterations can be shorter and longer).
STEP-BY-STEP GUIDE ON MOBILE APP HIPAA COMPLIANCE
Next, a list of results is compiled, and the priorities of those outcomes are determined based on customer opinions (or clients, customers – depending on the field). Finally, when each sprint is over, the team and customers evaluate the work and make changes for future sprints.
That is, instead of relying on legacy processes that often led to long delays, Agile emphasizes building the product quickly with short sprints and using end-user feedback to make improvements.
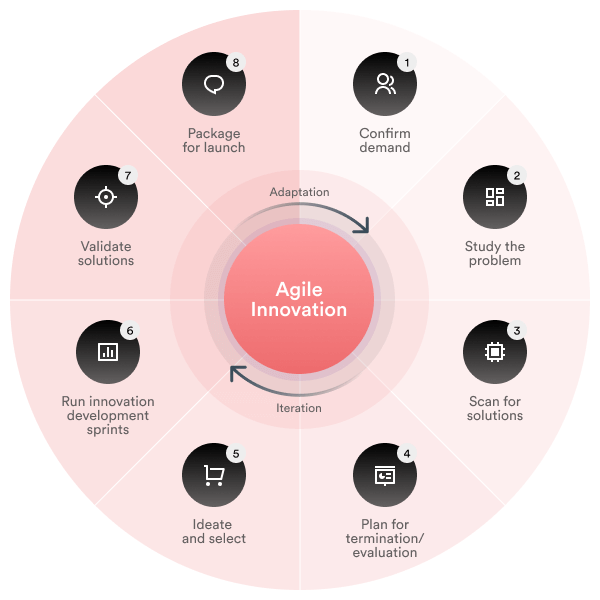
Operational communication between employees, and their vision of the situation at that moment, was placed at the center of the process – this allows a quick response and effective elimination of problems, as opposed to when employees strictly follow template instructions.
Thus, the connection between the customer/executor becomes stronger when the parties don’t go exactly according to the contract but rather, the circumstances.
Another practice of Agile is daily stand-ups. These check-in meetings unite team members to note progress toward sprint goals and identify any blocking or hindering factors. Each participant in such a rally should briefly discuss the work that has already been done, what they are currently doing, and what is preventing them from completing the next work phase.
Regardless of the specific application case, Agile helps companies move from a method where everything is carefully and diligently planned, to a technique that quietly breaks down those plans if necessary, immediately creating new ones and accepting changes.
What is Agility Healthcare?
In healthcare, most of today’s management, business planning, and information technology implementation processes aim to reduce the risk for organizations and are often inflexible to quickly adapt to new technological changes, resulting in incremental changes that fail to deliver much-needed transformation.
Digital innovations entrepreneur Martin Högl can confirm this – as he has encountered it in Germany. According to Martin, German healthcare is a highly conservative field.
You can learn more about thi from the CareMinds channel – The APP Solutions podcast. You’ll find other exciting guests there as well.
Agile in healthcare starts with ensuring patient satisfaction. At the same time, adopting Agile methodologies helps companies deploy functional applications quickly, accelerating flexible development processes.
READ ALSO:
PODCAST #1. CREATING A FUTURISTIC SURGICAL ROBOT
HOW TO MAKE EHR/EMR EPIC INTEGRATION WITH YOUR HEALTH APP
HOW TO MAKE A MEDICAL APP: THE ULTIMATE GUIDE
When to Use Agile in Healthcare?
Given the complexity and limitations, healthcare companies can benefit more from adopting an Agile methodology than other industries. Healthcare organizations are inherently complex adaptive systems. Multiple, medical and non-medical professions work with technology to meet the needs of virtually every patient who walks through their doors within an ever-changing regulatory and reimbursement environment, and with rapidly growing medical knowledge.
Agile does not dictate what medical teams should do. Instead, it offers guidelines to help teams decide how to prioritize work, communicate, and adapt to challenges along the way.
HEALTHCARE CYBERSECURITY: HOW TO PROTECT PATIENT DATA
In healthcare, Agile focuses on patient voices and developing the best solutions to satisfy those voices. To succeed, individual departments within organizations, such as business planning and information technology, must give their employees freedom and flexibility.

An Agile team comprises of clinicians, engineers, project and product managers, data scientists, and testers. Each team creates an iterative cycle to improve outcomes and increase value for patients, healthcare providers, and the system. At intervals, the team meets to review progress and identify bottlenecks and the means to address them. In addition, the team analyzes user experience to respond to feedback and promptly make revisions.
Teams start by discussing the “dream project” as the customer sees it. Then a start and finish line are formed – from what and to what they should come. And the points between these distances may undergo significant changes along the way, because when you bluntly follow a linear process, you risk falling behind your competitors, or simply getting a different result from what was planned.
KEY DIFFERENCES IN EHR VS. EMR VS. PHR: WHAT TO CHOOSE FOR YOUR HEALTHCARE ORGANIZATION
This approach no longer works in the dynamic marketplace that the healthcare industry has recently become. Instead, there needs to be constant communication between everyone involved in the process, even those who have not yet started or have already finished their part. Everyone involved, from developers to testers, from engineers to doctors, from the delivery to the marketing team, must be in close contact at all times to avoid unpleasant surprises.
Agile allows healthcare companies to start adapting and innovating effectively in the field of:
- Patient care
- Clinical workflows and digital health technology
- Organizational strategies
- Clinical Operations
- Pharmacology
- Insurance Medicine
Teams can use agile to redefine the model of care for patients, taking into account their goals and needs. The Agile approach provides the means to explore, integrate, and adapt to new and emerging scientific knowledge and tools, as well as the ability to respond to the changing needs and expectations of patients and families to create a truly adaptive, responsive system of care. Innovative healthcare organizations are using this Agile approach to deliver patient-centered care.

Practical Steps for Integrating Agile Principles into Healthcare Operations
Encouraging teams to be more efficient, flexible, and customer-centric in their workflows, collaboration, solutions, and products, Agile principles offer companies multiple benefits. They increase adaptability, enhance flexibility, speed up production, improve product quality, increase customer satisfaction, and boost the brand’s image. They might also support better resource allocation and minimize risks and operational costs. Here are the practical steps for integrating them into healthcare operations.
First and foremost, start with understanding Agile principles. There are 12 postulates that you should know.
Second, select those that suit your team, workflow, product, strategies, and current goals.
Third, start small and low. Adopt a step-by-step strategy to implement principles and assess their real impact on your company’s operational flow and productivity. Ensure it benefits your company without compromising your current progress and position in the market.
Fourth, prioritize patient-focused principles to improve care and treatment plans.
Finally, stay legitimate by meeting compliance and regulations. The agile principles must ensure that your workflows are legal and comply with the laws.
The Benefits of Agile in Healthcare
Such a work structure (if it is done correctly) promotes a number of advantages.
- Improving the quality of medical services – focusing on the patient’s needs. Now the patient can consult with a doctor without leaving home thanks to telemedicine. Patient monitoring and care are constantly being improved through adequate documentation in medical facilities.
- The flexibility of communication/reaction – Agile healthcare eliminates unnecessary correspondence and reduces the time for organization and coordination. Different departments that consistently relate to each other can communicate effectively, resulting in simplified mechanisms and innovations that were not even planned for at first.
- Introduces clear metrics, encouraging the team to self-organize, empowering it – all team members must clearly understand the scope of their responsibilities, which depends on their actions and on whom they depend (so there are no blockers and bottlenecks). KPIs are better tied to some kind of unit expression to make it easier to measure efficiency. Your staff must be trained to organize themselves and make decisions at critical moments.
- Innovations – when introducing a new process, going through the cycle faster always plays into your hands. For example, developing and testing a new drug will be much more effective with constant checking and correction, rather than blindly following a plan that may end up being very different from reality. Agile teams quickly respond to difficulties and lapses, correcting them promptly.
How To Make A Medical App: The Ultimate Guide
In moving to Agile, teams work directly with users for development and feedback, IT team members continue with initiatives rather than withdrawing from projects after the initial launch, and budgets and strategic plans remain as flexible as possible to accommodate the uncertainty inherent in the process. All of these initiatives have been woven into the fabric of the health systems using Agile methodology.
Teams do not follow prescribed practices or established tools, although they do use some organizational frameworks, such as Scrum, to plan their work. Prototypes, or minimally viable products, are prioritized to ensure early launch and experience; they are often initially deployed in a small area for improvement and data collection. Documentation in workflows, training materials, or code development is created as part of an innately collaborative process, fostering sustainability but with the initial goal of communication.
KEEP A PULSE ON EPIC APP ORCHARD AND HOW IT BENEFITS THE HEALTH SYSTEMS
Teams focus on vision and goals, both short-term and long-term, define key metrics and performance measures and engage in iterative work cycles. For example, teams change direction when data and user reports show that tools or services are not being used as intended initially, or when the user needs change.

THE APP SOLUTIONS – CUSTOM HEALTHCARE SOFTWARE DEVELOPMENT COMPANY
Implementation of Agile Principles: Step-by-Step Guide
How to implement Agile methodology in your medical institution? Here are some tips from McKinsey:
-
Define the goals – meet with the team leading the organization’s transformation into Agile. Then identify the overall strategic objectives of the enterprise and discuss how applying agile will help you achieve them. Plans may include targeted segment/market growth, improved value-based service models, and cost recovery opportunities.
-
Determine which part of your company is easiest to introduce Agile – for example, the development department. Start with changes there, gradually moving to more “conservative” teams.
-
Create a new model – identify the specific aspects that make up the stable backbone of your organization, then overlay dynamic capabilities and a model for agile teams and departments.
-
Introduce Agile gradually – start with general features and patterns and then refine those processes with each new iteration through feedback. Create space to learn and adapt in the field, then scale by moving target areas to a more agile model.
-
Improve – using the standard features of the methodology, use it in a way specific to your company.

Outcomes
Healthcare organizations can accelerate the introduction of new ideas and learning through the following key elements derived from Agile principles: using user-centered design to clarify the problems to be solved, key metrics, and potential solutions; empowering the team to quickly develop a usable prototype using a collaborative, disciplined approach and testing the initial implementation of early work; and adopting new ideas Agile includes testing and validation as an integral part of the product improvement process.
In this way, Agile innovation tangibly contributes to revitalization in healthcare by helping:
-
Multidirectional development of the industry as a whole
-
Shorten the lead time for product MVPs
-
Diversify the range of solutions by investing in new features or products
-
Improve efficiency and reduce costs through productivity
-
Respond quickly to customer/user requests and feedback
-
Increase transparency in both clinical and non-clinical areas
-
Qualitatively improve staff skills, promote staff autonomy
The APP Solutions builds any project based on Agile methodology because it has proven its effectiveness in communicating with clients and getting feedback from users. You can see the results of our work in the Portfolio. See also our case studies in the field of healthcare.
